Teenage acne is a common issue that can cause significant distress and self-consciousness during a crucial period of personal development. This skin condition is primarily a result of hormonal changes that happen during puberty, leading to an increase in sebum production and the subsequent blockage of pores. Dealing with teenage acne is crucial, not just because it can result in physical scarring but also because of its psychological effects.
Untreated acne can seriously affect a teenager’s self-esteem and social interactions, potentially leading to feelings of isolation, depression, and anxiety. Therefore, it’s vital to comprehend and effectively manage teenage acne to promote overall well-being during this critical phase of life.
Contents
- 1 What is Teenage Acne?
- 2 What are the Symptoms of Acne?
- 3 What causes acne in teens?
- 4 Types of Teenage Acne
- 5 Where do Acne Breakouts Happen?
- 6 How to Treat Teen Acne?
- 7 Which Treatment Option is Right for You?
- 8 How to Prevent Acne?
- 9 Myths and Facts about Teenage Acne
- 10 When to Seek a Dermatologist?
- 11 Conclusion
What is Teenage Acne?
Teenage acne, clinically referred to as acne vulgaris, is a skin ailment characterised by various types of skin lesions. These blemishes typically manifest on the face, back, and chest. During adolescence, hormonal shifts stimulate the sebaceous glands to increase sebum production, an oily substance that protects the skin. However, too much sebum can lead to the obstruction of pores, facilitating bacterial growth and the development of skin lesions.
Teenage acne is especially prevalent due to hormonal fluctuations during puberty. Elevated androgen levels, a category of hormones encompassing testosterone, prompt the enlargement and hyperactivity of sebaceous glands. This hormonal upheaval, in conjunction with other factors like stress and dietary choices, contributes to the widespread occurrence of acne during adolescence. It’s essential to note that while teenage acne is more frequently observed in males due to higher androgen levels, females can also experience this condition.
What are the Symptoms of Acne?
Acne symptoms can vary, but there are common signs to look out for. One main sign is the appearance of different types of blemishes, like blackheads (visible clogged pores), whiteheads (invisible clogged pores), red bumps, pus-filled pimples, painful lumps under the skin, and sometimes painful lumps filled with pus.
Alongside these visible symptoms, many individuals may also experience redness and inflammation around the affected areas. This redness results from increased blood flow as your immune system reacts to bacteria and dead skin cells trapped in your pores. Inflamed acne lesions can also cause tenderness or pain, especially when touched.
Another common symptom is increased skin oiliness or greasiness due to overactive sebaceous glands producing excess sebum. However, some individuals may also notice patches of dry, flaky skin, which can be a reaction to certain acne treatments.
In severe cases of acne, scarring can occur, leaving small depressions or raised areas of excess skin tissue. Seek professional medical advice if your acne symptoms are severe or causing distress, as early intervention can prevent physical scarring and alleviate psychological impact.
What causes acne in teens?

Teenage acne is typically attributed to several factors, further complicated by individual genetic predispositions.
Hormonal changes during puberty
One of the main reasons teenagers get acne is changes in their hormones. When teenagers go through puberty, their bodies start making more hormones, especially one called testosterone. These hormones tell the oil glands in the skin to make more oil, a natural substance that protects the skin. But if there’s too much oil, it can lead to acne.
Excessive sebum production
Excess sebum production is a key factor in acne development. While sebum is important for skin health, too much can cause issues. Hormonal changes during puberty stimulate sebum production. This creates an ideal environment for Propionibacterium acnes, which naturally resides on the skin but thrives in blocked pores. The resulting inflammation leads to red, swollen pimples, a hallmark of acne. Excessive sebum production plays a significant role in acne’s progression.
Clogged hair follicles and pores
Clogged hair follicles and pores contribute to acne formation. Accumulation of sebum (skin oil) and dead skin cells obstruct these structures, creating an environment for P. acnes bacteria to thrive, leading to inflammation and acne lesions. However, sebum production is not the sole cause of pore blockages. Improper skincare routines, comedogenic products, lack of exfoliation, diet, and stress play a role. Understanding these factors is crucial for effective acne management and prevention.
Bacterial presence
P. acnes bacteria, naturally present on the skin, can contribute to acne when hair follicles and pores are clogged. They produce enzymes and chemicals that inflame the skin and generate fatty acids from sebum, worsening inflammation. They can penetrate deeper in severe cases, causing painful nodules and cysts. Understanding the role of P. acnes is crucial for effective acne treatment.
Other contributing factors
Various other factors also contribute to the development of acne in teenagers, including stress, diet, genetic factors, and environmental influences.
Stress: While not a direct cause, stress can worsen acne by triggering hormone production and increasing sebum.
Diet: Controversial, but potential links exist between high-glycemic foods and dairy, causing insulin spikes and acne.
Genetics: If your parents had acne, your risk is higher due to genetic factors related to inflammation and hair follicles.
Environment: Pollution, high humidity, and exposure to oil or grease can exacerbate acne by boosting skin oil production. Recognising these factors is essential for acne management.
Types of Teenage Acne
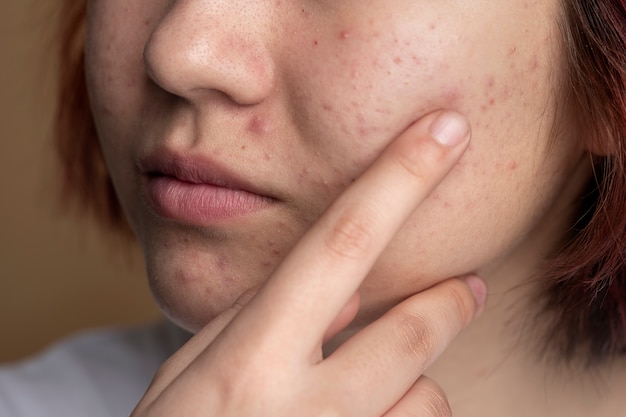
Teenage acne can present in various forms, each with its unique appearance and potential complications. Understanding these different types can help tailor effective treatment approaches.
Blackheads: These are small bumps that appear on the skin due to clogged hair follicles resulting from a combination of sebum and dead skin cells. The surface of these bumps appears dark due to oxidation, not dirt, as often misconceived. Blackheads can be managed by maintaining a consistent skincare routine, including gentle exfoliation to remove dead skin cells and excess oil.
Whiteheads: Similar to blackheads, whiteheads form when a pore becomes blocked by dead skin cells and sebum. However, the pore’s top is closed, making it white or flesh-coloured. Topical retinoids can effectively treat whiteheads by promoting cell turnover and preventing clogged pores.
Papules: These are small, hard, and often tender red bumps that signal inflammation or infection in the hair follicles. Reducing inflammation with over-the-counter treatments that contain salicylic acid, benzoyl peroxide, or a combination of both can be beneficial.
Pustules: If papules become filled with pus, they evolve into pustules. They are characterised by their red base and white or yellow tip. Pustules should never be popped, as it can lead to scarring or a deeper infection. Instead, the application of a spot treatment containing benzoyl peroxide can help.
Nodules: These are large, inflamed, and painful bumps that develop deep within the skin, often caused by a severe type of acne. Nodules may persist for weeks or months, and over-the-counter treatments are often ineffective. Their management typically requires prescription medications from a dermatologist.
Cystic acne: The most severe type of acne, cystic acne, forms when bacteria triggers inflammation deep within the skin, leading to large, red, painful, pus-filled cysts. If not treated properly, cystic acne can cause significant skin damage and permanent scarring. This condition generally requires a dermatologist’s attention and could involve treatment with oral antibiotics, isotretinoin, or hormonal therapies in female patients.
Where do Acne Breakouts Happen?
Acne breakouts commonly occur in areas of the body with a high concentration of oil glands. Here are the most prevalent locations:
Face: Acne is most common on the face due to the high density of oil glands. It often appears in the ‘T-zone’ (forehead, nose, and chin), where oil glands are particularly active.
Chest: The chest also experiences acne breakouts. Although it has fewer oil glands than the face, its thicker skin can trap more oil and dead skin cells, leading to breakouts.
Back: Referred to as ‘bacne’, back acne can be more severe due to the thicker skin and higher density of oil glands. Tight clothing and heavy backpacks can worsen it by causing friction and trapping sweat.
Shoulders: Acne breakouts on the shoulders are common, mainly due to the presence of oil glands and friction from clothing, especially in active individuals or those carrying heavy bags or backpacks.
How to Treat Teen Acne?
This part will explain how to treat teenage acne. You’ll learn about stuff you can buy without a prescription, medicines your doctor can give you, and some changes you can make.
Over-The-Counter Acne Treatments
Over-the-counter or OTC acne treatments are widely available and can effectively treat mild to moderate acne. These products work by reducing oil on the skin, speeding up the skin cell turnover process, fighting bacterial infection, or reducing inflammation – all of which can help prevent the formation of acne. Using these treatments effectively involves regularly and persistently applying the product(s) as directed by the package instructions.
Here are a few common OTC acne treatment ingredients:
Sulphur
Benzoyl Peroxide
Salicylic Acid
Alpha Hydroxy Acids (AHAs
In addition to OTC treatments, certain supplements and vitamins can also be beneficial for acne treatment:
Zinc
Vitamin A
Omega-3 Fatty Acids
Probiotics
Prescription Acne Medications
Prescription acne medications are often recommended for moderate to severe acne that doesn’t respond to over-the-counter treatments. It’s important to consult with a dermatologist or healthcare provider to determine the most suitable treatment for your specific condition.
Topical Retinoids: A derivative of Vitamin A, retinoids can unclog pores to allow other topical medicines to come into contact with the skin, reducing acne and improving the skin’s overall texture. Examples include tretinoin, adapalene, and tazarotene. Retinoids are usually applied at night and can cause dryness, redness, and increased sensitivity to the sun, so it’s recommended to use sunscreen during the daytime.
Oral Antibiotics: These treat severe or inflamed acne, such as cystic acne, by reducing bacteria and fighting inflammation. Examples include tetracyclines, erythromycin, and clindamycin. Long-term use is typically avoided due to the risk of antibiotic resistance. Side effects can include stomach upset, dizziness, and skin discolouration.
Isotretinoin: This is a potent medication used for severe, resistant, or nodular acne. It reduces the size of the oil glands, helping to prevent the clogging of pores and decrease bacterial growth. However, it can also have severe side effects, including dry skin, nosebleeds, muscle aches, and mood changes. More seriously, it can cause congenital disabilities if taken during pregnancy, so it’s important to use effective contraception.
Hormonal Therapy: This is often used in females to regulate hormones that can cause acne. Medications like oral contraceptives or spironolactone can reduce androgens, helping clear the skin. Side effects can include weight gain, breast tenderness, and blood clots.
Professional Acne Treatments

Professional acne treatments are another viable route, particularly if you’re grappling with severe or persistent acne that hasn’t responded to other treatment methods. Dermatologists administer these treatments, and can be effective.
Chemical Peels: Typically involving salicylic acid or glycolic acid, chemical peels exfoliate the skin deeper than most topical treatments, thus helping to unclog pores and remove dead skin cells. This process can also stimulate the growth of new, healthier skin.
Microdermabrasion: This technique uses a handheld device to gently remove the outer layer of the skin. It’s particularly effective for treating superficial acne scars and discolouration, providing a smoother skin texture.
Laser and Light Therapy: These therapies reduce the inflammation-causing bacteria on the skin and shrink the oil (sebaceous) glands, thereby reducing the amount of oil produced. Types of light therapy include blue light, pulsed light and heat energy (LHE), and photodynamic therapy (PDT).
Corticosteroid Injections: A dermatologist may inject a diluted corticosteroid to reduce inflammation and promote healing for large, painful acne cysts. These injections can also help prevent scarring.
Drainage and Extraction: Dermatologists use specialised tools to extract unresponsive whiteheads and blackheads. It’s crucial to have this procedure done by a professional to prevent possible scarring.
Which Treatment Option is Right for You?
Choosing the right acne treatment largely hinges on your acne’s severity and skin type.
Let’s consider a few scenarios:
Mild Acne (comprising mostly of whiteheads or blackheads): If you have an oily skin type with mild acne, over-the-counter treatments with active ingredients like salicylic acid or benzoyl peroxide may be adequate to manage your condition. You may also benefit from supplements such as zinc or omega-3 fatty acids.
Moderate Acne (frequent breakouts with a mix of whiteheads, blackheads and small pimples): For those with combination skin dealing with moderate acne, you might need a stronger line of treatment such as topical retinoids or oral antibiotics prescribed by a dermatologist, along with maintaining a routine with over-the-counter products.
Severe Acne (large, painful pimples or cysts): In cases of severe acne often associated with dry or sensitive skin, it’s crucial to consult a dermatologist. Prescription medicine like isotretinoin or hormonal therapy might be recommended. Professional treatments like microdermabrasion or light therapy could also be beneficial.
How to Prevent Acne?
Preventing acne often hinges upon implementing key skincare habits and lifestyle adjustments. Here are some effective strategies:
Gentle Face Cleaning Regime: Washing your face twice daily with a mild, non-soap cleanser can help remove excess oil and dead skin cells. Be sure to also wash after sweating heavily.
Avoid Over-Scrubbing: Scrubbing your face harshly can irritate the skin and worsen acne. Use your fingertips to apply the cleanser, and rinse with lukewarm, not hot, water.
Non-Comedogenic Products: Opt for oil-free or non-comedogenic skin products, including lotions, sunscreens, and cosmetics, formulated to avoid blocking pores.
Hands Off: Resist the temptation to touch your face, as doing so can spread bacteria and irritate already inflamed skin.
Nutrition and Hydration: Maintain a balanced diet of fresh fruits and vegetables. Hydrate adequately to help detoxify your body and keep your skin healthy.
Regular Exercise: Regular physical activity can help regulate your hormones and decrease inflammation, preventing acne. Remember to shower after exercising to wash away sweat and bacteria.
Adequate Rest: A good night’s sleep helps rejuvenate your skin. Chronic sleep deprivation can lead to stress, which may aggravate acne.
Stress Management: High stress levels can worsen acne. Incorporate stress management practices into your routine, such as meditation, yoga, or deep-breathing exercises.
Skin Care for Teenagers
To prevent and treat acne, maintaining a proper skincare routine is crucial. This usually involves cleansing, toning, moisturising, and applying sunscreen. Regular cleansing removes excess oil and dead skin cells, preventing clogged pores and breakouts. Toning balances the skin’s pH level and removes any leftover debris. Moisturising keeps the skin hydrated and prevents excessive oil production. Lastly, sunscreen protects against sun damage, which can worsen acne and cause scarring.
Here are some popular products that can be incorporated into your skincare routine to help treat acne:
Salicylic Acid Cleansers: Salicylic acid is a beta hydroxy acid that penetrates deep into your pores to eliminate excess oil and help prevent acne.
Benzoyl Peroxide Spot Treatments: These kill the bacteria that cause acne and remove dead skin cells from pores.
Retinoid Creams: Available over-the-counter and by prescription, retinoids speed up the skin’s cell turnover rate, helping clear pores and prevent breakouts.
Azelaic Acid Gels: Azelaic acid helps reduce inflammation and the growth of acne-causing bacteria.
Clay Masks: These absorb excess skin oil and help unclog pores.
Hyaluronic Acid Moisturisers: Non-comedogenic and lightweight, hyaluronic acid moisturisers hydrate the skin without clogging pores, making them suitable for acne-prone individuals.
Myths and Facts about Teenage Acne
There are several misconceptions surrounding acne, particularly about diet, hygiene practices, and lifestyle choices. Let’s debunk a few of these myths:
Myth: Eating Chocolate and Junk Food Causes Acne – While maintaining a healthy diet generally benefits your health (including your skin), there’s limited evidence to suggest that indulging in chocolate or junk food directly causes acne. However, some studies suggest that consuming a high-glycemic diet or dairy products could trigger acne in certain individuals.
Myth: Poor Hygiene Causes Acne – Acne isn’t a result of dirty skin. Overly scrubbing or harshly cleaning your skin can irritate it, which might worsen acne. The key is to adopt a gentle skin-cleaning regimen.
Myth: Lifestyle Choices Have No Impact on Acne – Contrary to this belief, certain lifestyle choices like lack of sleep, high stress levels, and certain medications can indeed worsen acne.
When to Seek a Dermatologist?
If your acne is causing distress or affecting your self-esteem, or over-the-counter treatments aren’t helping after two months, it may be time to consult a dermatologist. Dermatologists are experts in skin conditions, and they can determine the type of acne you have and the appropriate treatment. Here are a few signs that suggest you should seek a dermatologist:
Severe Acne
Acne Scars
Over-the-counter treatments aren’t working
Acne begins to clear but then comes back
You have acne and rosacea
Your acne is causing emotional distress
Conclusion
In conclusion, teenage acne is a common issue that can be managed effectively with appropriate knowledge and a well-rounded approach. It’s crucial to remember that acne is not a reflection of your hygiene or lifestyle choices but rather a complex condition influenced by various factors such as hormones, genetics, and stress.
While adopting a consistent skincare routine, maintaining a balanced diet, leading an active lifestyle, and managing stress can aid in controlling acne, it’s also important to seek professional help when necessary.
Consulting a dermatologist can provide personalised advice and treatment to manage acne based on your skin condition. With patience, persistence, and the right care, overcoming teenage acne is achievable.





